Low-income cancer patients older than 65 less likely to die in a hospital setting and more likely to choose hospice when providers prioritize communication, decision planning.
5:00 AM
Author |
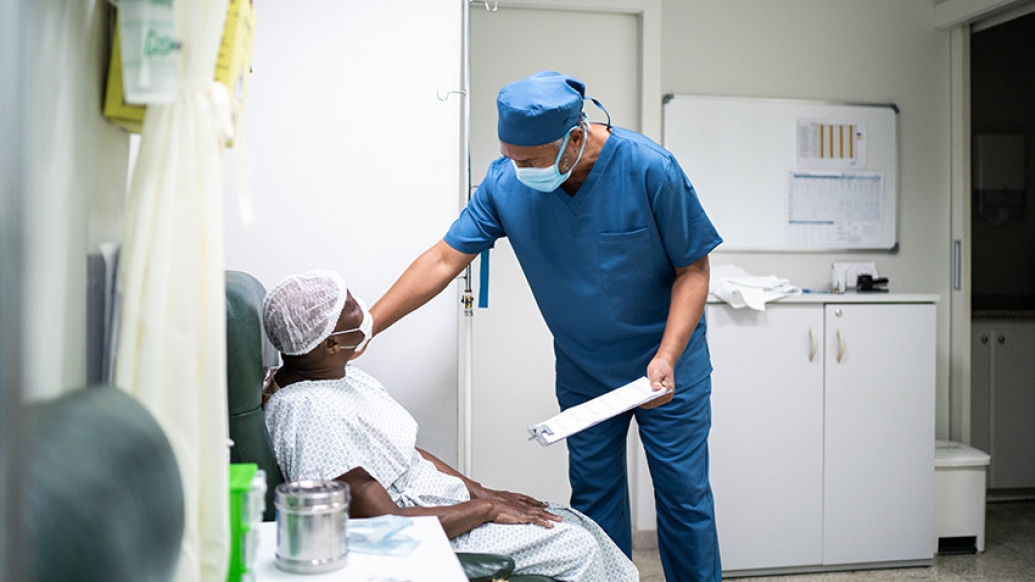
Cancer centers and/or health care systems that prioritize coordination and communication provide higher-quality end-of-life care for cancer patients who are eligible for both Medicare and Medicaid, University of Michigan researchers found.
Such "dual-eligible" people are more likely than those covered only by Medicare to experience aggressive treatment, like admission to the intensive care unit, shortly before they die. If, however, they receive care at a health care facility like a cancer center that values educating patients about their options and understanding their preferences about their end-of-life care, their chance of experiences that promote quality of life, like enrolling in hospice and dying in a setting other than the hospital, jumps significantly.
"We learned that health care systems can play a role in improving quality at the end of life for dual-eligible patients," said Lindsey Herrel, M.D., an assistant professor of urology at the University of Michigan Medical School and the first author of the study. "Where you receive care does matter to some degree. But there's certainly opportunity for better communication and shared-decision making at the end of life across the board for this population."
SEE ALSO: To Improve Medicare, Take Social Risk Factors into Account, Experts Say
About a fifth of people over the age of 65 who receive their health insurance through Medicare also qualify for Medicaid because of low income and minimal savings — and are considered dual-eligible as a result. That means Medicaid pays this population's monthly Medicare premiums as well as their copays.
However, dual-eligible Americans often face barriers to accessing health care outside of the cost of a doctor's visit. As primarily female people of color who have not attained a high school degree, many of them must manage systemic biases as well as socioeconomic disadvantages.
"We're talking about whether you can afford to put food on the table, whether you have the money to drive back and forth to the hospital," Herrel said. "All those things are real issues that people who are this low-income face."
Where you receive care does matter to some degree. But there's certainly opportunity for better communication and shared-decision making at the end of life across the board for this population.Lindsey Herrel, M.D.
Because of these hurdles, Herrel and her team hypothesized that well-coordinated care might be helpful for the dual-eligible population — especially at the end of life, when patients must make difficult decisions — and that where they received their care could affect its quality.
The researchers turned to several different datasets — including the Surveillance, Epidemiology and End Results (SEER) program, a common source of national cancer statistics, as well as health insurance claims from Medicare — to analyze close to 22,000 dual-eligible patients over the age of 65 who died of cancer.
They used seven metrics to measure whether quality of life seemed to be a priority for these patients and their medical teams, including whether they spent time in the hospital, the ICU or the emergency department in their last month of life and if and how long they were enrolled in hospice before dying (National organizations that issue guidelines around end-of-life care, including the American Society of Clinical Oncology, consider treatment that focuses on elevating quality of life versus curing disease, appropriate for patients with a prognosis of less than six months to live, and these measures reflect that perspective.)
When comparing designated cancer centers and integrated delivery networks — health care systems that emphasize education, communication, treatment planning and decision making — with health care facilities that don't fall into one of those two categories, the researchers found that dual-eligible patients received end-of-life care that emphasized quality of life at the former, across the majority of measures.
SEE ALSO: End-of-Life Care Remains Aggressive for People With Ovarian Cancer
Herrel says a possible explanation for the differences between types of health care systems could be that cancer centers and integrated delivery networks provide access to resources and an infrastructure that are better able to assess patient preferences when it comes to care at the end of life.
Going forward, though, a crucial step will be facilitating more of these conversations, regardless of the setting.
"It's really a matter of what does the individual patient and their family who's in front of you — What do they want? What do they need?" Herrel said. "They are difficult conversations to have from a provider standpoint to balance expectations and elicit patient preferences. But being a well-rounded clinician means you have to be able to have these discussions with patients and their families. Because without you helping them, they have to find other resources or are unable to get the information they want and need. So building ways we can foster communication is going to be the next best step."
Paper cited: "Intensity of end-of-life care for dual-eligible beneficiaries with cancer and the impact of delivery system affiliation." Cancer. DOI: 10.1002/cncr.33874

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





