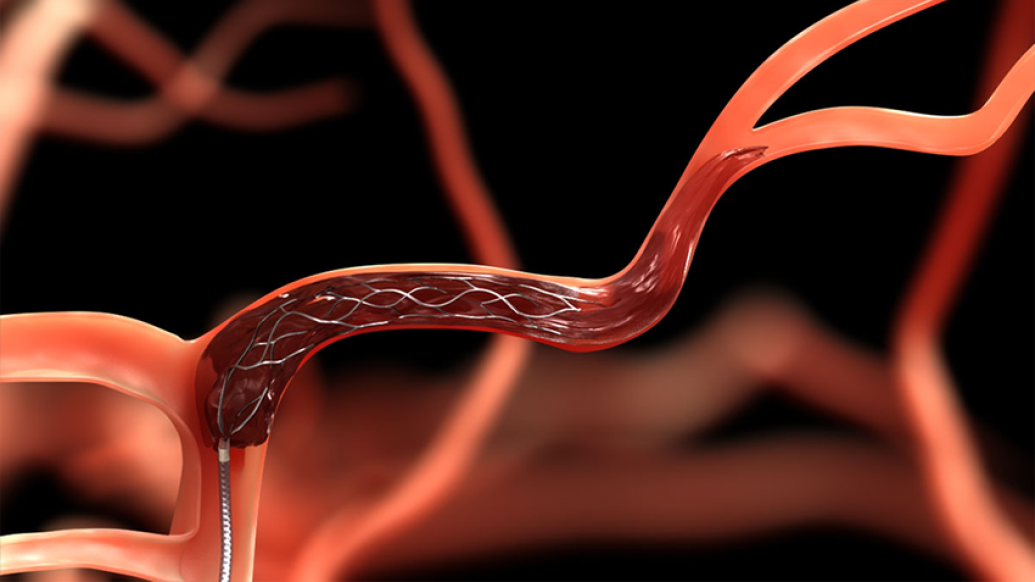
Plucking a blood clot from the brain with a tiny wire trap is proving highly effective when a stroke hits — with quicker recovery and improved long-term results.
12:49 PM
Author |
This article was updated on May 16, 2023.
Thrombectomy is a surgical procedure during which debilitating blood clots interrupting blood flow to the brain are ensnared and removed. By restoring blood flow to the brain, the aim is to minimize permanent brain damage and disability caused by stroke. This procedure often utilizes technology known as a stent retriever to clear the artery of clot and has helped many ischemic stroke patients achieve improved outcomes.
Inserted through an artery (typically in the groin), the collapsed stent can be expanded from inside a catheter once routed up to the brain's blocked blood vessel. A wirelike cage then "traps" the clot and ushers it out of the body. Catheter-based suction is also applied to improve the efficiency of the stent retrievers to open a blocked artery supplying the brain.
Using a 2-millimeter incision, the minimally invasive procedure takes about 60 to 90 minutes in most cases.
Stent retrievers can open blocked vessels 80 to 90% of the time — with "improved outcome" in 50 to 60% of patients after their discharge, says Neeraj Chaudhary, M.D., an associate professor radiology, neurosurgery, neurology and otolaryngology at the University of Michigan Medical School.
Growing usage and new indications
The first stent-retrievers were given approval from the United States Food and Drug Administration in 2012.
Although the technology has been available since then as part of the Neuro-Interventional portion of U-M's Comprehensive Stroke Program, it found wider adaptation nationwide after five studies on the procedure were published in 2015 in the New England Journal of Medicine.
This established thrombectomy as standard of care for patients suffering acute ischemic stroke with a blockage in one of the main arteries supplying the brain that were less than six hours out from when symptoms started. It was the first major advance in acute ischemic stroke therapy since intravenous tissue plasminogen activator (IV tPA), a clot busting medication, was shown to be effective in the mid-1990s.
Given that only a small fraction of stroke patients are eligible for thrombectomy based on the data from the 2015 clinical trials, ongoing efforts have been made to expand the number of people eligible for thrombectomy. In 2017, the DEFUSE 3 and DAWN trials published in the NEJM showed in a select subset of patients that thrombectomy could be beneficial up to 24 hours from when someone was last known to be well.
At the International Stroke Conference in February 2023, the SELECT 2 and ANGEL ASPECT studies suggested that even patients with larger strokes visible on imaging benefit from undergoing thrombectomy. Previously, there was concern that these patients may be too high-risk for the benefits of the thrombectomy to outweigh the risks. These two studies, both also published in the NEJM, showed markedly improved likelihood of good outcomes following thrombectomy as opposed to standard medical care.
“Ischemic strokes involving large vessel occlusion are often amongst the most disabling of strokes, and being able to offer thrombectomy to a larger and larger proportion of these patients is invaluable,” said Joseph Carrera, M.D., an assistant professor of neurology at U-M Medical School and medical director of the U-M Health Comprehensive Stroke Center. “I anticipate that the number of thrombectomies being performed could increase by up to 15-20% if eligibility from the recent large core thrombectomy trials are adopted nationwide.”
Ongoing research is being performed worldwide investigating use of thrombectomy in other populations of stroke patients to further increase the number of people that can receive this therapy. Despite the potential for thrombectomy to be performed further out from symptom onset, Carrera says, the importance of seeking medical care immediately upon identification of stroke symptoms remains critical.
“The earlier you get to the hospital, the more likely it is that you will be candidate for one of our acute stroke therapies, and the more likely it is that those therapies will work,” he said.

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!