For years, Maggie was questioning why she didn’t have the same stamina as her peers. A new diagnosis gave her peace of mind
8:59 AM
Author |

Thirteen-year-old Maggie Eggleston was growing frustrated that she was struggling to finish her cross-country races, play her violin or even put her hair in a ponytail.
Her mother, Debbie Eggleston, had also started noticing her daughter’s posture getting progressively worse after age 10. Being a physical therapist herself, she could tell something wasn’t right.
The family was referred to multiple physical therapists by their primary care physician to try to find answers with no success.
But after seeing a team at University of Michigan Health C.S. Mott Children's Hospital, Maggie Eggleston finally received a diagnosis: a rare and degenerative neuromuscular disorder called FSHD1.
It wasn’t the news the family was hoping for, but finally having an answer was a relief.
“There were so many things I was struggling with and didn’t understand why,” Maggie Eggleston said. “Now I know that it wasn’t anything I was doing wrong. It’s comforting to have an explanation.”
Finding an answer
At Mott, Maggie Eggleston saw physiatrist Angeline Bowman, M.D.. Upon first meeting, Bowman quickly saw that they were dealing with a neuromuscular disorder and knew tests should be run as soon as possible.
"For me, the telltale signs were the musculature of her shoulders and her saying that she struggled to hold air in her cheeks or blow a bubble," Bowman said. "These are common signs of certain neuromuscular disorders."
While waiting for test results, Bowman referred the Egglestons to Ava Lin, M.D., Ph.D., a Mott pediatric neurologist to ensure that all areas of care were covered.
All test results came back positive for FSHD1. The condition, which patients are born with and stems from a genetic mutation, causes the muscle cells to die off causing the muscles to decline in function. Symptoms can begin at any point in a patient's life, but for most, the condition doesn't start showing itself until adulthood. There is currently no cure for the condition, and it will progress throughout Maggie Eggleston's life.
"The trials that are being done are geared towards adults, so it will be a while before the research moves down to pediatrics," said Lin, who is helping provide Maggie Eggleston with proper treatment that minimizes symptoms. "It is important that we start paying attention to this in our pediatric populations since earlier onset means there is more time for the condition to progress. Being able to treat this earlier on in life would make a world of difference for the lives of these children."
Slowing the disease
FSHD1 comes with concerns for other areas of the body as well. These include cardiac, vision, and hearing concerns. Without proper maintenance and surveillance, the muscle breakdown can impact these areas causing less protection around the heart and lungs, vision loss, and hearing loss.
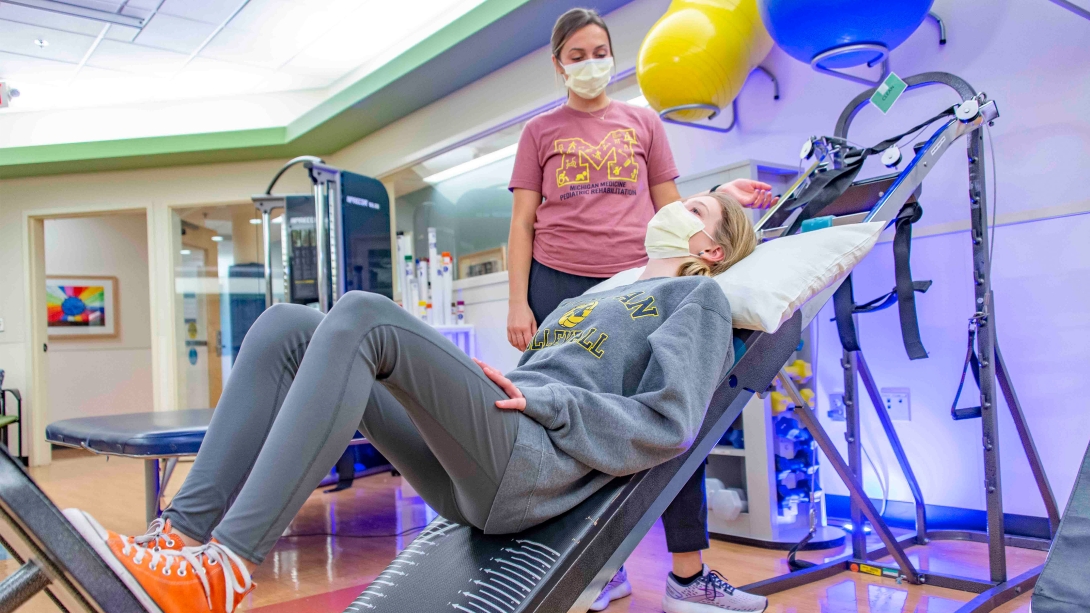
Until there's a treatment, Maggie will be working with her physical therapist, Paige Senn, to keep her muscles healthy and hold the symptoms at bay. Senn will be creating physical therapy plans to strengthen the teen’s muscles and slow their atrophy.
"It's important to be mindful of the types of muscle contractions she is doing so nothing is damaged further," Senn said. "A good gauge for the intensity of the exercise is to make sure she can hold a conversation during these activities."
Senn has created a physical therapy regiment that helps Maggie Eggleston find ways to do the tasks that she has struggled doing, such as pulling her hair up or playing the violin.

The goal is for the middle schooler to complete the tasks that she needs to in a way that works for her.
While it is rarer for symptoms of FSHD1 to start showing in adolescence, this care team has been working with FSHD1 patients in both adult and pediatric populations.
Looking ahead and spreading awareness
This spring, Maggie Eggleston graduates eighth grade and moves on to high school in the fall. While disappointed that some high school sports, such as cross-country, are no longer an option, she has found a love for musical theater and is determined to find a way to continue playing the violin.
"We wanted to share her story so other families don't feel alone," Debbie Eggleston said. "The condition is so rare and difficult to diagnose. We hope by bringing more attention to kids like Maggie we can start to find treatment."
The Egglestons say their biggest regret is that they didn’t receive a diagnosis sooner which would have allowed them to implement life changes to preserve the daughter's muscle tissues.
Since the diagnosis, Debbie Eggleston has joined many Facebook groups and organizations to help bring awareness to the need for research on FSHD1 in the pediatric population.
The mother-and-daughter duo encourage other families to see a specialist when something feels wrong and trust their gut. They also hope that pharmaceutical companies will start giving children with FSHD1 an opportunity to participate in clinical trials to move along the process of finding a treatment.
"We are always willing to see new patients and assess them," Lin said. "It is better that patients come to us with concerns that turn out to not be serious than let something unknowingly get worse over time."

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





