Family support helps baby and parents navigate heart failure and transplant
Mariana Lizcano’s grandmother and health care team — the “unicorns,” as her sister says — were key to the two-year-old’s recovery
5:00 AM
Author |
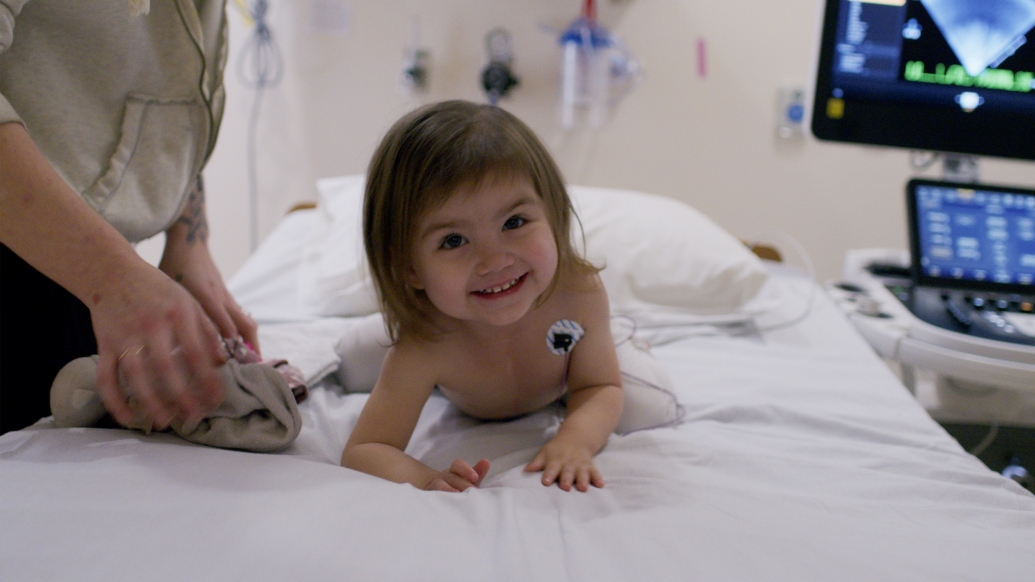
“Nap tiiiiiiime, Dad! Ahhhh!”
Mariana Lizcano squealed as her father, Juan, picked the two-year-old up and set her on his lap. She squirmed, sliding onto the floor, a sly grin on her face. The family’s husky ran behind the ottoman where Juan, Mariana and mother Jessica were sitting.
“Moah, go lay down, sit, sit, sit,” Jessica told the dog as she joined the fray, hoping for pets.
Mariana grabbed a board book off a shelf nearby and showed a picture to Juan.
“A turtle!” she yelped.
“It’s a whale,” Juan corrected gently.
Juan and Jessica were trying to do an interview about Mariana’s experience undergoing a heart transplant at University of Michigan Health C.S. Mott Children’s Hospital when she was less than a year old.
But as the Lizcanos know so well, life doesn’t pause just because there’s something important on your calendar. When Mariana began coughing and sleeping long hours, when a chest X-ray came back showing that her heart had swelled to 80% of her chest, when she needed to be flown by helicopter from Toledo to Ann Arbor for further evaluation, they made sure their daughter got the help she needed. Yet they also had a dog and another child, Mariana’s older sister Liliana, to take care of and rent to pay.
Understandably, they needed support. Luckily, they got it.
Mariana’s extensive care team — made up of cardiologists, nurse practitioners, dietitians, occupational therapists, physical therapists, social workers, surgeons and more — did everything they could to save the sassy little girl who’d found herself in heart failure. (“U-M treated us like family,” Juan said.)
Jessica’s mother, Wendy Holley, stayed with Mariana at Mott during the workweek over the five months she was hospitalized.
And at home in the town of Swanton, Ohio, Liliana provided hope for the whole family, believing with all her might that something magical would happen — that a unicorn would bring her sister home.
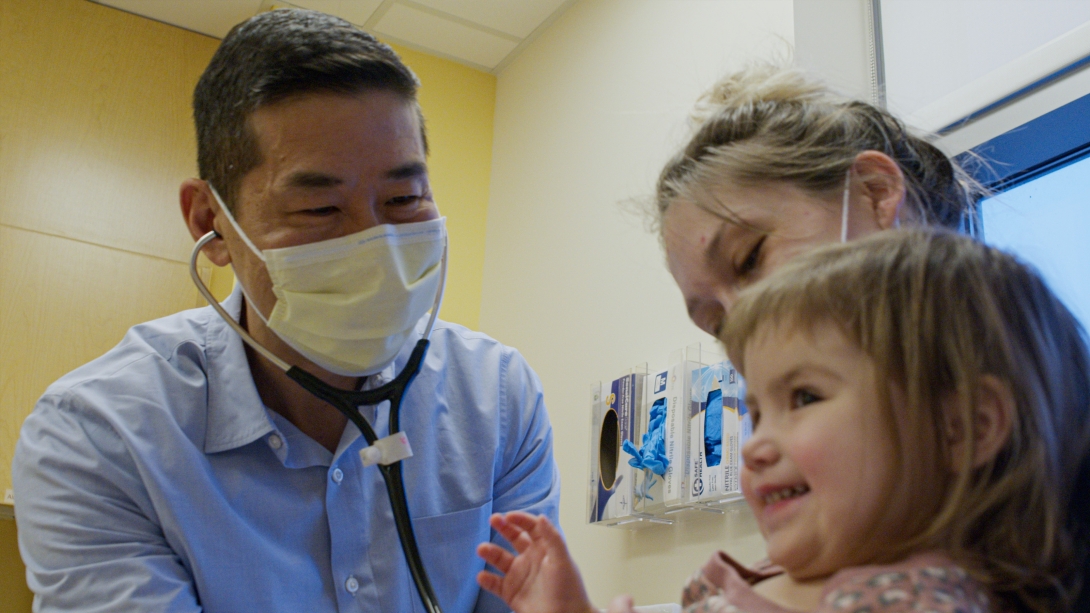
David Peng, M.D., is one of many providers on Mariana’s large care team.
“The pump wasn’t doing its job”
Mariana had arrived at Mott in a life-threatening state. She’d needed a ventilator and a breathing tube. Her providers gave her medications through an IV to support her heart.
Some children in heart failure eventually transition from IV medications to oral alternatives, an important step given the long-term side effects that can come with the IV treatments.
And at first, Mariana did indeed wean off the more intense drugs. But then she backslid. The time had come to consider more extreme measures, including a heart transplant.
Given the rarity of hearts available for transplantation in children — many families wait six months or longer for a compatible heart — and the lifelong need for medications and follow-up after transplant, the pediatric heart team takes the decision of whether to put a patient on the transplant waitlist seriously.
“We can’t pull new hearts off the shelf,” said David Peng, M.D., the director of pediatric heart failure and mechanical circulatory support at Mott and one of Mariana’s cardiologists. “People have said before that heart transplant is the answer to heart failure like the lottery is the answer to poverty. It’s not the best solution, and we’re always looking for better ways to get kids through heart failure without needing a transplant.”
A committee that includes members from all disciplines on the team discusses the benefits and drawbacks from each of their perspectives.
“As stewards of a new organ, we have to ask ourselves as a big team with psychologists and social workers and dietitians, will this organ do well in a new body?” said Vikram Sood, M.D., the surgical director for pediatric heart transplants at Mott. “Because if we don’t think that the family is going to have an opportunity to come to the hospital for the appropriate care, if the patient’s mental wellness and physical wellness won’t be otherwise cared for, then you can plug a new organ into someone but not have it do well, which is an extremely sad thing because that could have been used for someone else.”
SEE ALSO: A Birthday Gift with Heart: Healthy Tween Celebrates Her Transplant (michiganmedicine.org)
From Sood’s perspective, Mariana was a good candidate for transplant. She didn’t have other medical conditions, and the anatomy of her heart and its surrounding vessels didn’t make the operation more challenging, as it can for children with congenital heart defects.
“There wasn’t anything unusual outside the fact that the pump itself wasn’t doing its job,” Sood said.
Eventually, the decision was made: Mariana would go on the transplant waitlist.

As is evident by Juan Lizcano’s tattoo, family is one of his greatest values — and proved to be a crucial part of taking care of Mariana. Credit: Bob Feltz/Michigan Medicine
Structured support
Through all the uncertainty, Grammy Holley kept up a routine. Mariana woke up at 8 a.m. for blood draws. She had a bath every other night around 7 p.m.
“I didn’t know if we were going to be able to go home,” Wendy said. “I didn’t want Mariana to not be in the same routine as her sister. I wanted the flow to work for everybody.”
Wendy spent weekdays at the hospital so Juan could keep his job as manager of an auto repair shop, and he and Jessica could take care of Liliana at home. Grammy traded places with Juan and Jessica on the weekends, heading back to Swanton to be with Liliana while Mariana’s parents drove north.
As a retired nurse, Wendy was able to communicate with the care team on a different level than Juan and Jessica, especially during those first few months when Mariana was hospitalized.
“They didn’t mind if I challenged them, and I didn’t mind if they challenged me because everybody’s concern was Mariana, which was great,” Wendy said.
“Just by looking at her, you could tell the heart was pumping and doing everything it needed to do, that she was a whole different baby. Before we got the call that her heart was ready, she was going downhill. It’s amazing how fast things can change.”
- Juan Lizcano
Wendy could then relay the information she gleaned to Jessica and Juan.
“All of the words we couldn’t understand early on she would explain in her own way,” Jessica said. “And the emotional support she gave us — we wouldn’t have been able to do it without a third person.”
“A strong family structure is one of the greatest protective factors in pediatric heart transplant and strongly associated with a favorable outcome,” Peng said. “Mariana had a unique and amazing family structure that helped her to thrive.”
At home, Jessica and Juan were trying to quell Liliana’s fears that Mariana wouldn’t be coming home. FaceTiming from the hospital helped, so the older girl could see where her sister was. At one point, Liliana came up with the idea that a unicorn would save Mariana.
“Unicorns have magical powers, so Lily said a unicorn would bring Mariana home,” Jessica said. “I was like, ‘Oh, OK, well, that sounds wonderful. Maybe you’re right.’”
“They have a heart”
Mariana’s unicorn arrived on Aug. 6, 2021 — there was a heart for her.
“My dad had come pounding on the door saying ‘They have a heart! They have a heart!’” Jessica said. “We just lost it. It was so amazing.”
“There was a lot of relief and emotion of like, ‘OK, let’s get this done and let’s get back to normal life,’” Juan said.
When the couple crept into Mariana’s room to see her after her operation, they realized her foot was warm for the first time. Her face was pink instead of white.
“Just by looking at her, you could tell the heart was pumping and doing everything it needed to do, that she was a whole different baby,” Juan said. “Before we got the call that her heart was ready, she was going downhill. It’s amazing how fast things can change.”
After surgery, Liliana had asked how the unicorn put the heart in her sister.
“I remember Lily saying, ‘So she’s saved, she’s saved?’” Jessica recalled. “And I said, ‘Yes. She’s OK.’”
When Mariana arrived at the Lizcanos’ apartment in Swanton for the first time in five months, she couldn’t believe how many toys were waiting for her.
SEE ALSO: Heartbeat Songs Offer Young Transplant Patients Special Gift (michiganmedicine.org)
“When we were in our first place, she was in a bassinet, so that’s all she really knew,” Jessica said. “And then she comes home and gets to have a home and a family and normal things. So it was really wonderful.”
The family still had hurdles to navigate. Mariana needed to take immunosuppressive medications on a rigid daily schedule to prevent her immune system from rejecting her new heart. For the first year after transplant, she had to eat through a feeding tube, using a slightly thickened formula that made it easier for her to keep food down and decreased the risk of food going into her airway.
“For a lot of our kids who have been hospitalized and intubated for a long period of time, their strength and endurance decreases,” said Amanda Peck, O.T., an occupational therapist who worked with Mariana at Mott. “They’re trying to keep up with their eating skills like they typically would, but they don’t have the stamina. We’ll see coughing and choking, sometimes some vocal cord impairment, and food will end up in their airway instead of in their belly, so the thicker formula helps with that.”
As Mariana transitioned to more solid foods, there were other lifestyle modifications to remember. She couldn’t eat fish or eggs that were runny because of their higher risk of bacteria that could make her sick. In fact, the care team sent her parents home with a literal book’s worth of information about how she would need to live to avoid illness.
There were some rocky moments, but as the Lizcanos built stronger relationships with the outpatient care team they were now working with, everyone felt more confident.
“It’s a lot, especially for new, young parents,” said Meg Zamberlan, N.P., an advanced practice nurse at Mott who works with the Lizcanos. “But they’re doing fantastic now. They know when to call about Mariana’s symptoms. They know about her medications. They get her labs done. It’s going great.”
“Meg is my favorite because she doesn’t feed me only the good stuff,” Jessica said. “If something’s going down, she’s gonna sit there and she’s gonna tell me, but she’s also going to say, ‘But this is what we’re going to do about it.’ I love that. It’s fine if you give me a bad thing — but tell me how we’re gonna face it.”

Juan and Jessica Lizcano recall a funny moment from Mariana’s transplant experience. Credit: Bob Felts/Michigan Medicine
Mariana is two years old now. She loves orange juice and the Trolls movie and cleanliness. Her favorite words are “Why?” and “No!” She insists on doing the same things as Liliana, whether it’s getting the same color drinking straw at lunch or copying her sister’s dance moves in Grammy’s garage. The only sign that she underwent a transplant is the small scar on her chest.
“This is why I love doing what I do because our team gets to be there at the time of greatest need and help patients through the most critical periods,” Peng said, “and then continue to follow them if they’re fortunate enough to leave the hospital, see them grow up, go to school, play sports and just be a kid. A lot of times, we only see them a couple times a year in person, which is what we aspire to.”
“I look at her and I think about how glad I am that she’s here, that she can reach all these little milestones,” Wendy said. “We’re just so blessed.”
The care team was able to record the beats of Mariana’s old heart and encase it in a teddy bear that Wendy has kept. There’s a difference in the rhythms, Jessica says. Mariana’s original heartbeat was faster but much more subtle.
“The new one is a little slowed down,” Jessica said, “but more like, ‘I’m here. I’m here.’”

Health Lab
Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.
Media Contact

Public Relations
Department of Communication at Michigan Medicine
Stay Informed
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!
Featured News & Stories
Rx Kids linked to reductions in preterm births and low birthweights, fewer NICU admissions

Collaboration with community child care centers creates innovative research tool

Teenage patient receives treatment for papillary thyroid cancer

Teens need private time with doctors, but many aren’t getting it

A smarter helmet for the smallest patients
