Findings will help shape next steps in partnership between Detroit public schools and U-M school mental health outreach program.
9:27 AM
Author |

Even before the COVID-19 pandemic, serious mental health concerns impacted a significant portion of students in Detroit public schools, a new report shows.
More than half of student respondents in the Detroit Public Schools Community District had experienced symptoms of anxiety or depression, and an alarming 23% had seriously considered attempting suicide within the past year, according to a pre-pandemic assessment conducted by the DPSCD in collaboration with the University of Michigan Transforming Research into Action to Improve the Lives of Students (TRAILS) program and Youth Policy Lab.
The large-scale survey of more than 15,000 Detroit students, staff and families showed that against that backdrop, the DPSCD is committed to improving student well-being: all stakeholders voiced a desire to increase resources and training to better equip the district with effective and equitable student mental health services.
The needs assessment was the first step in a multiyear partnership between U-M and DPSCD that supports a pillar of the district's Blueprint 2020—the whole-child commitment. The collaboration will focus on student mental health with the goal of providing effective services in all 100-plus DPSCD schools. This aligns with the district's commitment to social and emotional development of its students in addition to physical health and academic readiness.
Like Podcasts? Add the Michigan Medicine News Break on iTunes, Google Podcast or anywhere you listen to podcasts.
Surveys completed by more than 11,000 Detroit students (grades 8-12), nearly 3,500 staff and 800 families provided data about risk and protective factors, access and barriers to care, student symptoms of depression and anxiety, satisfaction with available resources and attitudes about mental health. Findings will help to inform and evaluate the impact of future programming for students, staff and families.
"We recognize that the ability of students to take full advantage of educational opportunity requires that we create a foundational culture of health and wellness throughout each and every one of our schools," said DPSCD Superintendent Nikolai Vitti. "This assessment provides an unprecedented view of the well-being of the district and the priority needs identified by our community."
A survey effort of this size and scope is unprecedented and required extensive collaboration among DPSCD, TRAILS and the Youth Policy Lab.
TRAILS is a school mental health program designed to increase youth access to evidence-based mental health services. It provides professional development, resources and implementation support to school partners in effective practices that are appropriate for the school setting, such as cognitive behavioral therapy and mindfulness. The program has formally partnered with 350 schools statewide, reaching an estimated 90,000 students.
SEE ALSO: Personalized Screening to Identify Teens with High Suicide Risk
The U-M Youth Policy Lab is a partnership between the Ford School of Public Policy and the Survey Research Center at the Institute for Social Research and brings significant expertise to the initiative in school-based program evaluation.
Results from the needs assessment indicated that DPSCD students may experience unique mental health vulnerabilities. Many of those surveyed had experienced trauma and significant mental health concerns including suicidal ideation—the act of thinking about, considering or planning suicide.
The survey also found:
-
Rates of depression and anxiety symptoms, and suicidal ideation among DPSCD students far exceeded national averages.
-
23% reported having seriously thought about attempting suicide in the past year.
-
31% reported thoughts of suicide or self-harm in the past two weeks.
-
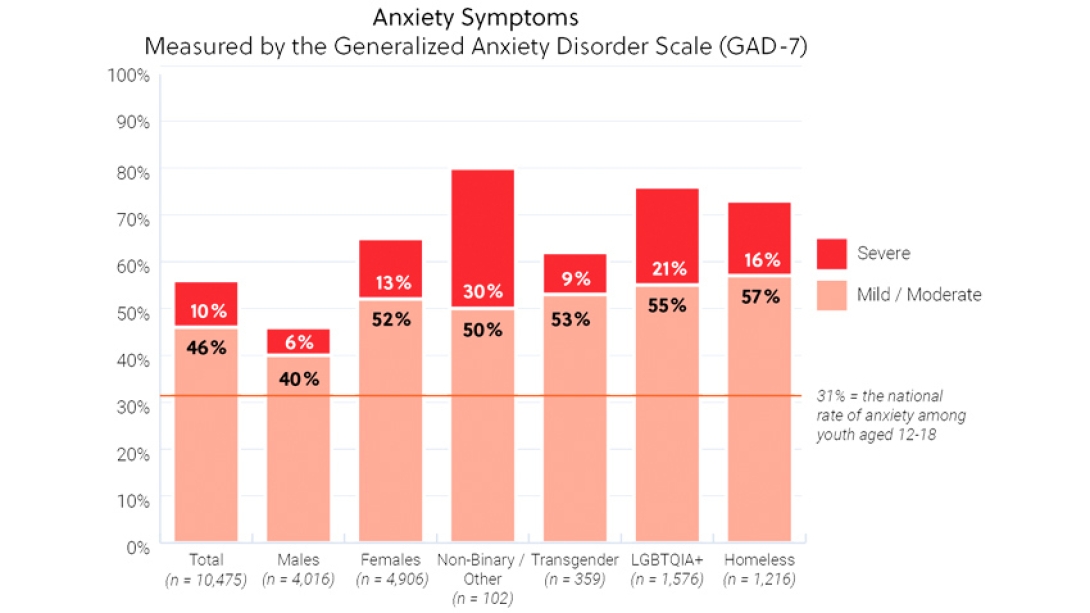
56% reported symptoms of anxiety.
-
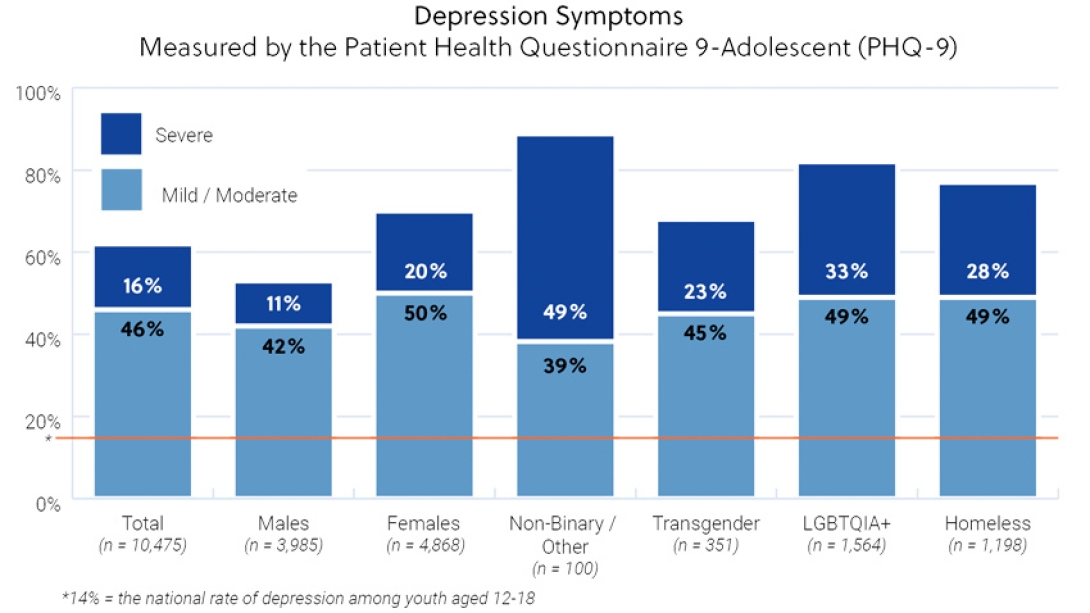
62% reported symptoms of depression.
-
Depression and anxiety symptoms were found not to impact students equally: Girls had higher rates of depression and anxiety than boys.
-
Nearly half of sexual and gender minority youth reported suicidal ideation.
-
Academic stress was the top mental health concern identified by students, followed by anxiety, depression and family stress.
-
A substantial number of students with symptoms of anxiety and/or depression reported not having ever accessed any school- or community-based mental health support services. The most common barriers to seeking mental health services cited included a preference for coping with difficulties on their own, a belief that available services would not be helpful and embarrassment/shame/stigma.
-
Students with depression, anxiety and exposure to trauma were more likely to report chronic absenteeism and difficulties completing schoolwork or studying. Rates of disciplinary involvement were also significantly higher among students with depression, anxiety and exposure to four or more traumatic events.
"The findings made it clear that DPSCD students were experiencing high levels of need around mental health even before COVID-19," said Robin Jacob, Ph.D., co-director of the Youth Policy Lab and an associate research professor in the U-M Institute for Social Research. "Given the disproportionate impact of the pandemic on communities of color, the need for mental health support for Detroit students is even greater now. The district's focus on mental health is key as students navigate their mental health needs related to the twin pandemics of COVID and systemic racism."
Despite reporting a high level of burnout, DPSCD staff universally reported a strong desire to help their students who are struggling, and they, along with administrators and families, overwhelmingly voiced a need for additional resources and training to ensure they are equipped to provide effective student mental health support. Teachers and administrators were most interested in training in social and emotional learning, while student support staff (e.g., counselors, social workers, nurses) hoped to strengthen best practices to support students affected by anxiety and depression.
Informed by survey findings, TRAILS is now collaborating with the district to implement responsive programming, and already nearly 4,000 DPSCD staff have attended districtwide TRAILS trainings on understanding and supporting student mental health needs and effective self-care strategies. Additional programming will commence this year and next spanning three tiers of student support: universal prevention, targeted intervention and suicide risk management.
One strategy that is central to the TRAILS model and will span all three tiers of programming is to leverage the school and community resources that are already in place, rather than creating solutions that are reliant on external funding or personnel.
"We believe that those best positioned to sustainably support the healthy growth and development of young people in any community are the very individuals living and working alongside those youth, particularly adults working in schools who are trusted by, and committed to, their students," said Elizabeth Koschmann, Ph.D., TRAILS program director and an assistant research scientist in the Department of Psychiatry at Michigan Medicine.
"By equipping schools to provide evidence-based mental health services, students impacted by mental illness, trauma exposure or environmental stressors will be more likely to develop coping strategies that will lead to better school engagement and performance and improved mental health across the lifespan."
Also core to the TRAILS model is acknowledgement of the role racism plays in driving inequities in mental health and health care access. For many BIPOC, a history of medical racism combined with pervasive social stigma create additional barriers to mental health help-seeking and treatment beyond those that are more logistical, such as difficulty scheduling or high costs.
SEE ALSO: Fewer Deaths Among Adults Who Got Extra Support as Suicidal Teens
"Efforts to address mental health needs in DPSCD must include work to eradicate these more systemic barriers," Koschmann said.
Long term, the U-M and DPSCD partnership is anticipated to help students participate more meaningfully in school, improve attendance and academic performance, engage in fewer noncompliant and high-risk behaviors, remain in school longer, and ultimately benefit more fully and equitably from the academic opportunities available to them in their Detroit schools.
TRAILS acknowledges the many organizations that funded this work: Blue Cross Blue Shield of Michigan Foundation, Centers for Medicare and Medicaid Services through the Michigan Department of Health and Human Services, The Children's Foundation, Community Foundation for Southeast Michigan, Detroit Medical Center Foundation, Ethel & James Flinn Foundation, George B. Storer Fund at The Miami Foundation, The Jewish Fund, Metro Health Foundation, Michael & Betsy Mackey Family, Michigan Health Endowment Fund, National Institute of Mental Health, Prosper Road Foundation, Susan M. Wellman Family Fund, U.S. Department of Education, and the U-M Department of Psychiatry.
The report does not include the experiences of students who declined to participate or who were absent during the survey window. DPSCD, TRAILS and the Youth Policy Lab acknowledge that those are likely some of the students at highest risk and that there's an underrepresentation in the needs assessment of students about whom experts might be most concerned.

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





