Clinical trials show longer survival in patients with diffuse midline glioma treated with ONC201; study also explains underlying mechanism of the drug’s success
10:00 AM
Author |
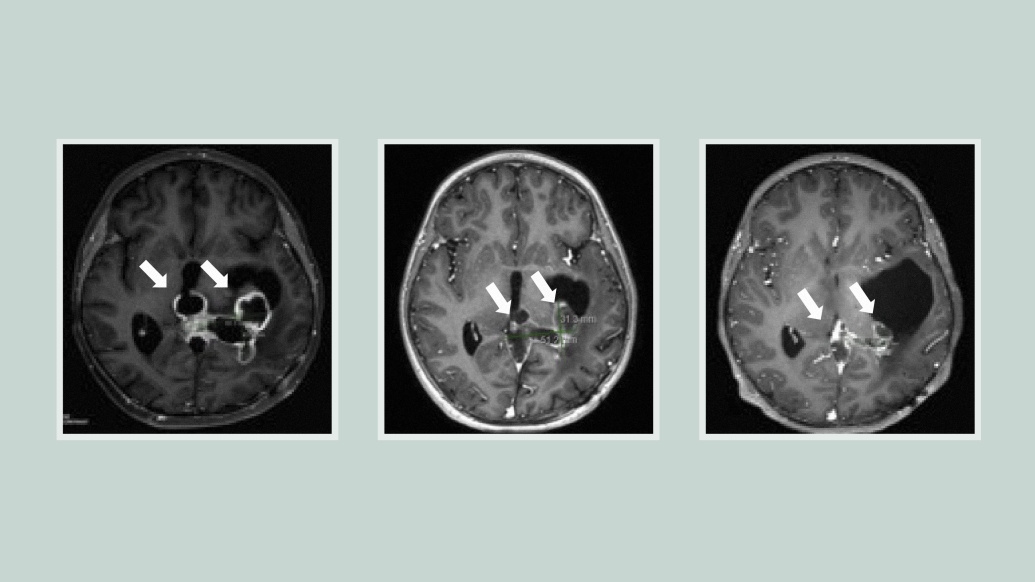
For the first time, researchers have found a potential drug candidate that improved outcomes for patients with a type of childhood brain tumor for which there are no effective treatments.
The compound, called ONC201, nearly doubled survival for patients with diffuse midline glioma or diffuse intrinsic pontine glioma, compared to previous patients.
The findings are reported by an international team of researcher led by the University of Michigan Health Rogel Cancer Center and the Chad Carr Pediatric Brain Tumor Center.
In addition to reporting on the results of two early stage clinical trials, the paper reveals the underlying mechanisms behind the compound’s success in these tumors.
The paper is published in Cancer Discovery, a journal of the American Association for Cancer Research.
Diffuse midline gliomas including DIPG with a mutation called H3K27M are particularly aggressive, with an overall survival rate of 11-15 months.
These tumors are most frequently found in children and young adults. The only available treatment is radiation, and even that is difficult as the tumors are located amid brain regions with critical functions.
“It’s an incredibly difficult tumor to treat,” said senior author Carl Koschmann, M.D., associate professor of pediatric neuro-oncology and clinical scientific director of the Chad Carr Pediatric Brain Tumor Center at Michigan Medicine.
“Prior to this study, there have been more than 250 clinical trials that have not been able to improve outcomes. These results are potentially a major crack in the armor,” explained Koschmann, who is also a pediatric neuro-oncologist at U-M Health C.S. Mott Children’s Hospital.
In two clinical trials testing ONC201 in a total of 71 patients with H3K27M-mutated diffuse midline gliomas, the median overall survival was nearly 22 months for tumors that had not recurred at the time of enrollment. Almost a third of the patients lived longer than two years.
ONC201 took an unusual path to a clinical trial.
Initially designed to target dopamine receptors, which are upregulated in many different tumors, researchers saw that the drug passes the blood-brain barrier, one of the biggest challenges to designing drugs for brain tumors.
Initial trials in glioblastoma were not successful, but a small number of patients with DMG that carried the H3K27M mutation had more promising results. Without understanding why it worked better in these patients, a phase 1 trial was started in children and young adults with H3K27M-mutated DMG.
Meanwhile, Koschmann and co-author Sriram Venneti, M.D., Ph.D., were trying to figure out what was happening in these tumor cells.
Through the trial, they collected cerebrospinal fluid from patients.
They used this fluid to analyze metabolic changes and found ONC201 got into the tumor cells and affected mitochondria. Patients who responded to the drug had an increase in a metabolite called L-2HG produced by tumor cells.
SEE ALSO: Spinal fluid sampling used to track treatment response in pediatric glioma
Koschmann called the finding “very much unexpected.”
The team found that increased L-2HG reversed tumor defining epigenetic signals causing tumor cells to differentiate more and divide less. The longer patients were on ONC201, the more tumors exhibited these epigenetic reversals.
“This could explain why this patient population was responding so well to the drug, because it had this specific epigenetic abnormality that could be turned off by ONC201. The tumors have an epigenetic change caused by the H3K27M mutation and ONC201 metabolically undoes that change,” said Venneti, associate professor of pathology and pediatrics and scientific research director of the Chad Carr Pediatric Brain Tumor Center at Michigan Medicine.
Additional clinical trials are currently underway, including testing ONC201 in combination with other therapies.
Researchers at U-M’s Chad Carr Pediatric Brain Tumor Center are also continuing to look at ways to overcome resistance to ONC201 by using drug combinations.
Koschmann notes that even a near-doubling of survival is not enough for families of patients with this diagnosis, as the tumor remains very lethal. But he hopes this first step will lead to bigger leaps in the future.
“For now we have this patient population that didn’t have a drug before, and now we see many of the tumors responding. We have a platform to build on and we can also explain why it’s working,” he said.
“We are really excited about this study and envision ONC201 becoming standard of care for these patients in the near future,” Venneti said.
Additional authors: Abed Rahman Kawakibi, Sunjong Ji, Sebastian M. Waszak, Stefan R. Sweha, Mateus Mota, Matthew Pun, Akash Deogharkar, Chan Chung, Rohinton S. Tarapore, Samuel Ramage, Andrew Chi, Patrick Y. Wen, Isabel Arrillaga-Romany, Tracy T. Batchelor, Nicholas A. Butowski, Ashley Sumrall, Nicole Shonka, Rebecca A. Harrison, John de Groot, Minesh Mehta, Matthew D. Hall, Doured Daghistani, Timothy F. Cloughesy, Benjamin M. Ellingson, Kevin Beccaria, Pascale Varlet, Michelle M. Kim, Yoshie Umemura, Hugh Garton, Andrea Franson, Jonathan Schwartz, Rajan Jain, Maureen Kachman, Heidi Baum, Charles F. Burant, Sophie L. Mottl, Rodrigo T. Cartaxo, Vishal John, Dana Messinger, Tingting Qin, Erik Peterson, Peter Sajjakulnukit, Karthik Ravi, Alyssa Waugh, Dustin Walling, Yujie Ding, Ziyun Xia, Anna Schwendeman, Debra Hawes, Fusheng Yang, Alexander R. Judkins, Daniel Wahl, Costas A. Lyssiotis, Daniel de la Nava, Marta M. Alonso, Augustine Eze, Jasper Spitzer, Susanne V. Schmidt, Ryan J. Duchatel, Matthew D. Dun, Jason E. Cain, Li Jiang, Sylwia A. Stopka, Gerard Baquer, Michael S. Regan, Mariella G. Filbin, Nathalie Y. R. Agar, Lili Zhao, Chandan Kumar-Sinha, Rajen Mody, Arul Chinnaiyan, Ryo Kurokawa, Drew Pratt, Viveka N. Yadav, Jacques Grill, Cassie Kline, Sabine Mueller, Adam Resnick, Javad Nazarian, Joshua E. Allen, Yazmin Odia, Sharon L. Gardner
Funding for this work is from National Institutes of Health (R01-NS119231, R01-NS124607, R01-NS110572, R01-CA261926, 1UM1HG006508, CA192427, U24-DK097153), Department of Defense (CA201129P1), University of Michigan Chad Carr Pediatric Brain Tumor Center, The Evans Family, ChadTough Defeat DIPG Foundation, Catching Up with Jack, Pediatric Brain Tumor Foundation, Prayers From Maria Foundation, Michael Miller Memorial Foundation, Morgan Behen Golf Classic, Yuvaan Tiwari Foundation, Sontag Foundation, Alex Lemonade Stand Foundation, Hyundai Hope Foundation, Research Council of Norway (187615), The South-Eastern Norway Regional Health Authority, The University of Oslo, Oncoceutics, Inc., Chimerix, Inc., Making Headway Foundation, Gustave Roussy Foundation Pediatric Campaign, Imagine for Margo Charity, National Research Foundation of Korea (2022R1C1C1011998), DGIST Start-up Fund (2021050001), University of Michigan Taubman Institute
This work was supported by these Rogel Cancer Center Shared Resources: Experimental Irradiation and Preclinical Molecular Imaging
Disclosure: None
Paper cited: “Clinical efficacy of ONC201 in H3K27M-mutant diffuse midline gliomas is driven by disruption of integrated metabolic and epigenetic pathways,” Cancer Discovery. DOI: 10.1158/2159-8290.CD-23-0131

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!





