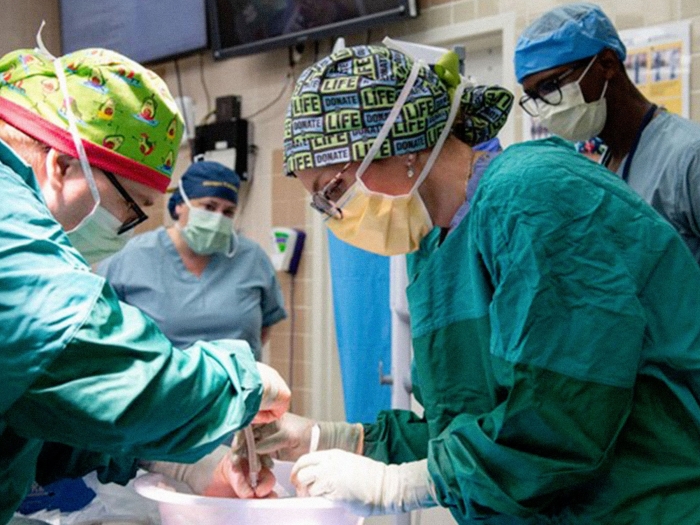
Studying data from hundreds of thousands of surgical cases in Michigan has made surgery safer, and recovery smoother, for patients across the state.
7:00 AM
Author |

Darrell Campbell Jr., M.D. used to get Christmas cards from patients whose lives he'd saved with kidney, liver or pancreas transplants. He'd get hugs and high-fives when they came in for appointments.
SEE ALSO: Curing Health Care with a Dose of Big Data and Common Sense
He gleaned satisfaction from every operation that went well, and from seeing young surgeons launch their careers after learning in the University of Michigan hospital's operating rooms.
But the patients he cares for these days don't call or write. They don't say hello in the hospital halls. They don't even know his name.
And yet, his work touches tens of thousands a year, making operations safer, surgical teams more prepared and recoveries smoother.
Campbell leads one of the largest data-driven quality improvement efforts in all of surgery, the Michigan Surgical Quality Collaborative, or MSQC, which helps surgical teams improve patient care. For the past decade, it has been the silent force behind a dramatic shift in surgical safety and better patient outcomes in Michigan.
"In my surgical career, we could really see a tangible benefit from what we did in virtually every patient," Campbell says. "But in population health efforts like MSQC, no one knows that you've helped them. They don't know that they were spared getting an infection in the hospital, or that their operation was performed in a way that's consistent with the same operation done on a patient a hundred miles away. But we're able to make a difference for hundreds or thousands of patients at a time."
A team effort
Just like any surgical team, MSQC is not a one-man show.
Campbell directs a team of 2,000 surgeons, nurses, data experts and others from 73 hospitals around Michigan. Together, they created a massive cooperative effort with funding from the state's largest insurer, Blue Cross Blue Shield of Michigan, and based out of the U-M Institute for Healthcare Policy and Innovation.
Each year, they collect 137 different types of data about 50,000 operations performed at participating hospitals, from the patient's weight to the exact drugs used during the operation.
The team's publications are causing a ripple effect for patients nationwide.
For instance, the team just published results from their efforts to reduce surgical site infections after colectomy surgery, or removal of part of the bowel. Infections dropped the more often teams followed a MSQC bundle of anti-infection protocols, and so did costs — at a rate in Michigan faster than the nationwide decrease during the same time period.
In another new paper, the team showed how complications from surgery more than doubled the cost of a patient's care and ate into a hospital's profit margin.
What we rely on is a spirit of collaboration. It's measurement to improve, not measurement to judge.Darrell Campbell Jr., M.D.
A new way of doing things
Campbell started down the road of improving surgery through shared data as chief medical officer of the U-M Health System, beginning in the late 1990s. He saw what VA hospitals had started to do: examining data from a national electronic health record system and acting on it.
SEE ALSO: How 'Love' and a Landmark Paper Improved Health Care
Unlike the VA hospitals, though, he knew most surgical centers in the U.S. don't have a way to share records securely and electronically — and even if it was possible, competitive pressures would stand in the way as facilities tried to stay afloat in Michigan's downturned economy.
If things were going to get better for patients at non-VA hospitals, he realized, it would take a lot of trust, technology and time.
Primary care doctors were already starting to do the same thing in their sphere. But they had so much work to improve management of common chronic conditions that surgeons weren't yet on the radar. Yet, nearly half of American medical care is related to surgical procedures.
So Campbell spearheaded U-M's participation in a surgical quality improvement project that started with three hospitals and grew to hundreds nationwide. The American College of Surgeons now runs the project. The effort won him a national award for patient safety. But in 2005, the opportunity arose to harness BCBSM funding and launch a statewide effort involving a few dozen hospitals.
Because a statewide initiative can be nimbler than a large national one, Campbell calls MSQC a real "boots on the ground" approach. A key part of its success, he says, has been cultivating a culture of trust and familiarity among participating teams through regular conference calls and meetings. He also credits responsive customer service from MSQC staff, who work directly with the nurses who spearhead data collection and reporting at each hospital.
"What we rely on is a spirit of collaboration — that we're not going to use the quality information to award trophies or put up billboards about who's the 'best in the state,'" he says. "It's measurement to improve, not measurement to judge. We treat the data confidentially, and share findings among our participants — including helping outliers understand how their practices or results differ from those around the state, and how they can change."
Continued growth
More hospitals have joined over the years, as MSQC attained a special status as a federal Patient Safety Organization. The kinds of operations that MSQC focused on grew, from general surgery, to vascular surgery and now gynecological surgery. Most recently, interventions to reduce inappropriate hysterectomy use, and infections among those who do opt for surgery, have rolled out for hospitals' use.
More tellingly, no hospitals have dropped out. More will join in the coming year. And other states, including South Carolina, Tennessee and Illinois, launched similar efforts with funding from local Blue Cross Blue Shield subsidiaries.
"The medical professions tend to be adversarial with big third-party payers, but we have the same goals of better quality and lower cost, and more appropriate use of care with fewer complications," says Campbell. "Through efforts like MSQC, we can work together productively with them."
The next challenge, he says, is connecting surgical quality improvement efforts with pre- and post-surgical care and linking up with quality improvement efforts in primary and nonsurgical specialty disciplines.
MSQC's rich data set, with records from more than 420,000 operations, can help drive such programs. For example, U-M has launched an effort based on MSQC data to help surgical patients reduce their risk of complications by undergoing pre-surgery "prehabilitation," which includes exercise, quitting smoking and emotional factors.
An additional effort draws on evidence from MSQC and other sources to help improve opioid painkiller prescribing after surgery.
Another challenge is to help hospitals improve the value of care for surgical patients — reducing cost and improving quality. Even if it costs more upfront, higher-value care will ultimately mean fewer repeat hospital stays, and less time in nursing homes and the emergency room, Campbell says. This is in line with Medicare and other insurers' move to change the way care is paid for to focus on value.
"It's a fertile field, and there's still a lot we can accomplish that can have a great impact on a lot of people," Campbell says.
So even if MSQC doesn't get Christmas cards from the patients its work touches, "We are learning from our data and acting on our data across a broad spectrum. For me, that brings a satisfaction of a different sort."

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!