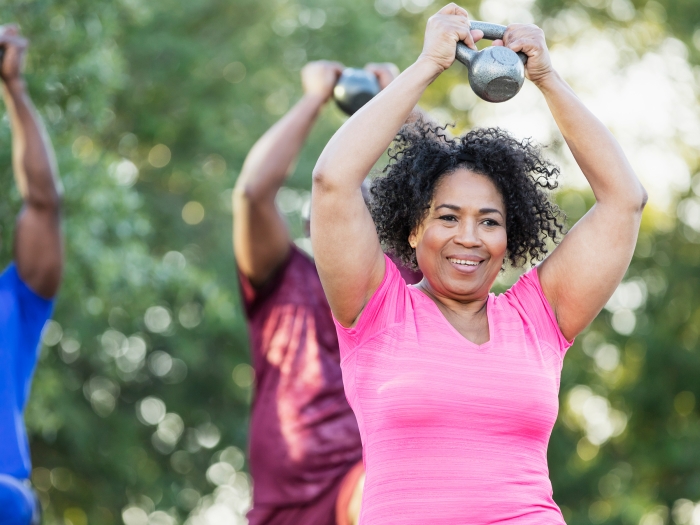The future of free preventive care and health screenings rests in the hands of judges and lawmakers – but for now, patients can keep getting them
1:35 PM
Author |

Updated June 24, 2024 to reflect the Fifth Circuit Court of Appeals ruling on June 21.
The best things in life are free. Or so the saying goes.
And for the last 14 years, some of the best things for your health have been free too – like screenings to look for early signs of cancer, diabetes, depression or other problems, and tools to help people stop smoking, reduce their risk of heart disease or prevent serious infections.
You might not have noticed it, but you haven’t had to pay out of your own pocket for many of these for more than a decade.
And the number of preventive services that you can get without spending money has grown over that time. That’s because new research can show what works best for finding or preventing future problems in people of certain ages, or with certain conditions.
But now, the future of this free-to-you coverage hangs in the balance, because of a court case working its way upward from Texas to the Supreme Court.
Nothing has changed for patients yet. Right now, these kinds of care are still available without cost, even after a June 2024 court ruling.
But that could change in future depending on how the court case goes. Some or all patients could have to start paying again – even if research shows that they really could benefit.
Two of the top national experts on this topic are University of Michigan professors who study the clinical, equity, financial and legal impacts of American health care. One – a physician – helped design, implement and evaluate the no-cost preventive services provision. The other – a lawyer – is an expert in the legal issues surrounding this case that could potentially effect over 150 million Americans.
Both want more people to be aware of what’s going on and what the outcome of the legal challenge might mean for those who currently received these services at no cost.
“This case holds the potential to create a barrier to potentially life-altering screening tests, but there is a potential one-line legislative fix that could preserve cost-free access,” said A. Mark Fendrick, M.D., a professor of internal medicine at Michigan Medicine and director of the Center for Value-Based Insurance Design.
He and U-M Law School professor Nicholas Bagley, J.D., are concerned that the court case could essentially result in a “freeze” on free preventive services, which could mean fewer people get them because of what it will cost them.
But they have also raised the possibility of a “fix” that states and Congress could enact to keep that from happening for some or all Americans.
The potential freeze
The court case in question, called Braidwood vs Becerra, focuses on the part of the Affordable Care Act that requires most private health insurance companies and plans that people buy through national or state marketplaces to cover the full cost of certain preventive health care services.
This means patients pay nothing for the screenings, tests and types of prevention-oriented health counseling that have earned top recommendations for specific groups of people.
The requirement started in 2010 with a list of a few dozen items, which will still be covered no matter what the ultimate court ruling is. The list has grown to more than 90 items over the last 13 years, as new research showed which preventive care gives the most benefit for people of certain ages or with certain health risks. Items added since 2010, and changes to the original items, are what’s potentially affected by the court case.
Fendrick and his team have compiled a quick-reference list with details about how the court case might apply to each one, and published an article in Health Affairs Forefront about it. The team has also compiled a full policy brief on the subject.
Three examples:
- Back in 2010, screening tests to look for early signs of colon cancer were free for people aged 50 to 75. Two years ago, that expanded to people age 45 to 49. If the Braidwood ruling is upheld, insurance companies could stop making such screening free for the over 20 million Americans between 45-49 years of age.
- Back in 2010, free screening for hepatitis C virus wasn’t on the list. But as ongoing research showed the power of new medications that can clear that infection and prevent liver failure, in 2020 all adults up to age 79 became eligible for a free screening test to see if the virus is lurking silently in their bodies. If the current Braidwood ruling stands, no-cost HCV screening would not be required.
- Just recently, mammograms for women over 40 got the preliminary stamp of approval that could lead to them becoming free every other year – just like mammograms for women over 50 have been since 2010, based on a 2009 recommendation. As a result, the 22 million women between the ages of 40-50 might have to pay out of pocket for their breast cancer screening if the courts agree with the plaintiffs.
Why is this happening?
The Texas case was filed by health providers who oppose a 2019 requirement that patients – most of them gay or bisexual men – receive free access to medications that can prevent them from getting infected with HIV, the virus that causes AIDS.
Even though these providers don’t offer HIV-related care themselves, they filed to block anyone from getting it for free. They based their case on a legal argument about the way that some of the experts who recommend preventive services are appointed to their posts. Bagley explained it in this short video.
If the plaintiffs ultimately prevail in court, that could ‘freeze’ the entire list of free services as if it were 2010 again. Only those patients who were eligible for a free service 13 years ago would be able to get it, and no new people could be added based on new research.
“It would be like setting the nation’s medical clock back and not allowing it to advance,” said Fendrick.
The case boils down to a legal argument about the three ways that preventive services can become free under the Affordable Care Act.
One is to earn a rating of A or B for specific types of people from an independent panel of experts called the U.S. Preventive Services Task Force, which evaluates research and only gives its top recommendations when the evidence of benefit is strong. In addition to endorsing new services, the Task Force regularly updates its recommendations based on the most up to date research, as was the case for the colorectal cancer screening and hepatitis C virus examples.
“The Texas judge specifically ruled that because the members of the USPSTF are not appointed in the right way, they can't make constitutional decisions, and thus their A and B recommendations that employers and insurers are supposed to follow in providing zero-dollar coverage for preventive care are unconstitutional and invalid,” said Bagley in 2023.
“The judge ruled that it doesn't just apply to the plaintiffs who filed the lawsuit opposing just one recommendation for prevention of HIV transmission, but it applies to everybody and to all USPSTF recommendations,” he added at the time. “And that, of course, set off an effort by the federal government to pause his decision, while appeals could work their way to the U.S. Supreme Court.”
But in the new June 2024 court ruling by the Fifth Circuit Court of Appeals, Bagley posted on X (formerly Twitter), "The Fifth Circuit sided with the challengers when it came to PSTF. Its members supposedly have the authority to bind private parties, but those members weren't properly appointed. So PSTF's decisions aren't really official at all; they're just, like, its opinions. There's a bit of a silver lining, however...for now, the PSTF-related injunction applies only to these plaintiffs, not across the whole country."
So, he said, the status quo for ACA coverage of all USPSTF-recommended services stands. But this could change.
Fendrick also reacted to the new court ruling, saying, "The Fifth Circuit ruling maintains the status quo (for now) for the highly popular ACA policy that eliminates out-of-pocket costs for many high-quality preventive services - for over 200 million Americans - that have been proven to prevent diseases or to detect conditions while they’re still treatable. This decision provides a welcome reprieve to a possible Braidwood ruling that would limit the removal of cost-sharing to only those preventive services recommended by the USPSTF before the passage of the ACA in 2010, would have enormous clinical and equity implications."
The other two ways a service can become free are to get approved by a federal agency called HRSA for services specific to women or children, or in the case of vaccines to get recommended by a panel of advisors to the federal government called ACIP.
The court case may not affect these two paths, though there is some chance it could. Birth control is an example of a preventive service that could return to having cost-sharing for patients if HRSA-approved services are included.
Bagley's thread of posts on X/Twitter ended with, "So we're in for more litigation before this case makes it up to the Supreme Court. How much more? Well, probably a couple of years. Litigation is slow! For now, the status quo holds, but it looks like the preventive services mandate may be in trouble down the line."
The potential fixes
It could take a couple of years for the Braidwood case to get to a Supreme Court ruling. In the meantime, some states such as Michigan have said that they will still require cost-free coverage of these services for insurance programs that they have power over – but that doesn’t include many insurance plans run by companies and paid directly by employers.
Large insurance companies have also said that they will continue to honor the free-to-you coverage for services that previously earned USPSTF A or B ratings, while the case moves through the courts.
But it is uncertain whether plans will cover new recommendations – such as the one to start breast cancer screening at age 40 instead of 50 – at no cost while the case is being decided.
If the courts ultimately rule that USPSTF recommendation of a service isn't sufficient because of the way its members are named, insurers won’t have to cover the full cost of any services recommended after 2010. Even if they do, they could delay changing their coverage instead of having to make the change within a year of a new recommendation, which they must do now.
Fendrick worries that this will mean costs for some people -- for instance, people with high-deductible health insurance plans or people who fall into a group that gets newly added to an existing recommendation.
According to a recent consumer survey, 37% of adults said they “definitely” or “probably” expect to delay or avoid heath care due to potential costs following the ruling, and at least 2 in 5 adults said that they are not willing to pay for preventive services that are currently fully covered by the ACA.
“We need some confirmation or guarantee that will remove any confusion and let individuals know that they will continue to receive these important preventive services for free,” he said. “The crux of this issue is that according to the Texas ruling, you have to be an agent of the federal government to make policy, and the USPSTF is not a government agency.”
One way to fix this would be for Congress to pass a one-line provision recommending or requiring that the federal Secretary of Health and Human Services approve any recommendations that receive an A or B from the USPSTF. Since the secretary is a federally appointed role, their approval would hold the force of law.
Given that members of both political parties have previously expressed support for this part of the Affordable Care Act, this may be possible, Fendrick said.
It’s not a perfect solution, but it may have bipartisan appeal since every president has the ability to appoint an HHS Secretary, who could decide not to approve recommendations to cover specific services if no-cost coverage of such services is opposed by members of the president’s political party.
This same scenario of politics getting mixed up with preventive health could happen if the courts decide that HRSA-approved services for women and children and ACIP-recommended vaccines cannot be considered separately from USPSTF-recommended services. That’s what the people who filed the court case in Texas tried to convince the judge to rule.
“If future court rulings bring the preventive services selected by these two additional organizations back into consideration, then the likelihood of bipartisan support to pass legislation to assure no cost coverage of these essential preventive service becomes even less likely,” Fendrick said. “And that would increase the risk of barriers to care and resulting inequality.”

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!