Nearly 2 decades after a groundbreaking discovery, Arul Chinnaiyan wins a prestigious cancer research award.
2:45 PM
Author |

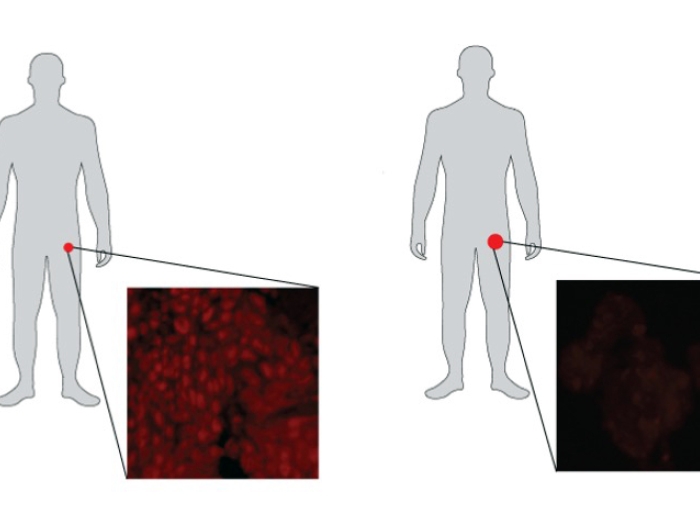
In 2005, Arul Chinnaiyan, M.D., Ph.D., and his lab found what they realized was the "on switch" for prostate cancer. A gene regulated by androgens called TMPRSS2 fuses with a transcription factor called ERG to trigger the development of prostate cancer.
This gene fusion was the first ever identified in solid tumors. In the nearly two decades since, the Chinnaiyan lab has refined its discovery, understanding how the hormone androgen regulates this gene fusion and developing a urine-based screening test to better detect prostate cancer.
MORE FROM THE LAB: Subscribe to our weekly newsletter
For this work, Chinnaiyan, S.P. Hicks Professor of Pathology and Urology at Michigan Medicine, was named the winner of the 2022 Sjöberg Prize, awarded by the Royal Swedish Academy of Sciences, which also awards Nobel Prizes.
This is the sixth time the Sjöberg Prize has been presented. It was established by businessman Bengt Sjöberg to promote scientific research primarily focused on cancer, health and the environment. The Royal Swedish Academy selects the laureates and the Sjöberg Foundation provides the $1 million prize funding.
"One of the things that made the TMPRSS2::ERG gene fusion unique and exciting is that it is found only in prostate cancer, not in normal prostate tissue," said Chinnaiyan, director of the Michigan Center for Translational Pathology and a member of the University of Michigan Health Rogel Cancer Center.
This allowed the lab to significantly improve on the traditional prostate specific antigen, or PSA, test to detect prostate cancer. They combined the gene fusion, PSA and one other prostate cancer marker into a urine test called MyProstate Score, or MPS. Studies have shown this test is more accurate than a standard PSA test for predicting cancer as well as predicting aggressive prostate cancer. The test is commercially available.
In addition, the Chinnaiyan lab has used the technology behind this discovery to uncover gene fusions in other common cancers. They continue to investigate how these fusions can be targeted for treatment.
Here, Chinnaiyan reflects on his discovery and shares what it means to win the Sjöberg Prize.
What did you think when you first heard you won the Sjöberg Prize?
Chinnaiyan: To receive an email from the Royal Swedish Academy of Sciences was a pleasant surprise, especially considering the isolation during these pandemic times. I was even more thrilled to hear I was selected for the 2022 Sjöberg Prize. It is a great honor to be selected for this award and to follow in the footsteps of the luminaries who have received this award in the past.
What has been the impact of the gene fusion discovery?
Chinnaiyan: The discovery of recurrent gene fusions in prostate cancer was certainly a stunning finding back in 2005. Before that time, it was thought that gene fusions and translocations were major drivers of hematological cancers and rare soft tissue tumors. But we had found these gene fusions in high prevalence in a common solid tumor, that being prostate cancer.
The TMPRSS2-ETS fusions that we identified ended up being exquisitely specific biomarkers of prostate cancer that can be detected in prostate needle biopsies and non-invasively in the urine of men with prostate cancer.
After our discovery, a number of recurrent gene fusions were identified in subsets of other common solid tumors, including lung cancer, breast cancer and melanoma, among others. The finding of recurrent gene fusions in prostate cancer also opened up the use of transcriptome or RNA-sequencing in precision oncology efforts.
How will you use the award money?
Chinnaiyan: As this award recognizes our discovery of recurrent gene fusions in prostate cancer, I plan to use this support to fund our efforts to directly and indirectly therapeutically target these and other cancer-causing transcription factors. As transcription factors have been challenging to develop drugs against, we plan to approach this from a variety of angles.
Again, I'm grateful to theRoyal Swedish Academy of Sciences and the Sjöberg Prize Committee for recognizing our work.
Like Podcasts? Add the Michigan Medicine News Break on iTunes or anywhere you listen to podcasts.

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!