An orthopaedic surgeon discusses some debates in foot and ankle care and the importance of personalized medicine in the field.
5:10 PM
Author |
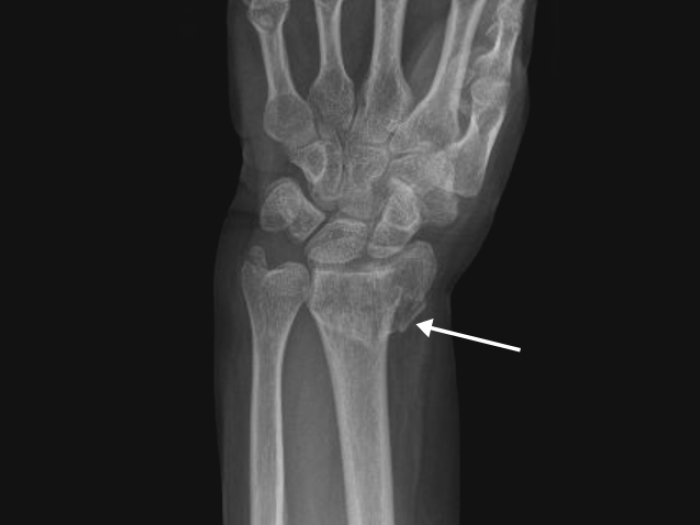
As more people get back to physical activity that waned during the onset of the COVID-19 pandemic, foot and ankle surgeons are busier than ever. The subspecialty sees a wide array of complex injuries, from sprains and tendinitis to Lisfranc fractures and ankle dislocations.
There are tried-and-true methods for specific injuries, but some issues have dozens of treatment options. And, over time, many of the methods once deemed standard may change or become obsolete as medicine evolves.
Paul Talusan, M.D., associate professor of orthopaedic surgery at Michigan Medicine, discusses the debates over treatment in foot and ankle surgeries:
What are some debates currently circulating in foot and ankle surgery?
For every ailment we see, there are, and should be, conversations about how we should treat them. For example, there are over 100 operations described for bunions. There is scientific evidence to support good results for a lot of these operations, which means that there is certainly no perfect operation for a bunion. One of the reasons for this is that there isn't just one kind of bunion out there; they come in various shapes and sizes. The most important thing is that surgeons adhere to sound orthopaedic principles when addressing a bony deformity. Regardless of the technique that is used, adherence to sound orthopaedic principles – cutting the bone where it needs to be cut depending on the severity of the bunion, shifting the bone to the necessary spot and maintaining the correction with stable hardware – should have a favorable result.
ALSO SEE: For orthopaedics, women in leadership look to transform the field
Some other controversies that exist include minimally invasive versus open surgery, ankle fusion versus ankle replacement and Lisfranc fusion versus Lisfranc open reduction and internal fixation (ORIF). As with bunions, there are different opinions about the best option, and there is scientific evidence to support all sides.
How are the debates around foot and ankle surgery affecting clinical practice and outcomes?
In clinical practice, surgeons are using a combination of their training, clinical acumen, evidence-based medicine and patient input to inform how they treat certain conditions. In terms of outcomes, if a surgeon is seeing less-than-ideal results with a surgical technique, they will usually change their approach to treating that condition. One of the wonderful things about these debatable topics is that these conversations often lead to more research questions and inspire us to keep innovating and trying to make these topics less controversial.
What are some proposed solutions?
The short answer to solving some of these controversies is to have higher quality scientific studies with large numbers of patients and multiple surgeons from several institutions. Some of the studies on which we base our practice are of extremely high quality. However, some of what we do is based on evidence that is not as developed as we would like. That is certainly the case in very complex patients with unique foot issues, and the answers to their problems are not found in a textbook or in the literature.
ALSO SEE: Achilles injuries skyrocket as America returns to normal. Here's how to handle them
In addition to scientific studies, it is also important that we maintain a line of communication among us surgeons and can discuss complicated issues. The American Orthopaedic Foot & Ankle Society and American Academy of Orthopaedic Surgeons have done an excellent job in providing opportunities that allow surgeons to educate each other.
Why is personalized medicine important for foot and ankle surgery?
Personalized medicine is important because every patient is unique. Going back to the topic of bunions, every bunion is like a fingerprint – no two are identical. Although there are many similarities from one bunion to another, a surgeon must be vigilant in analyzing the morphology of the bunion to approach it uniquely and achieve the best result for that patient.
That approach does not just apply to bunions or just foot and ankle surgery. There are many areas of surgery and medicine that now use personalized or precision medicine to guide their practice and optimize health outcomes for patients. It is another tool foot and ankle surgeons can use to ensure patients can return to function.
Talusan is one of many Michigan Medicine faculty members and residents involved in the 2021 AAOS Annual Meeting. For more information on the meeting: https://michmed.org/O5L7o

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!