The deadly third wave of the 1918 flu shows what can happen when society prematurely returns to pre-pandemic life, a medical historian cautions.
10:13 AM
Author |

Picture the United States struggling to deal with a deadly pandemic.
State and local officials enact a slate of social-distancing measures, gathering bans, closure orders and mask mandates in an effort to stem the tide of cases and deaths.
The public responds with widespread compliance mixed with more than a hint of grumbling, pushback and even outright defiance. As the days turn into weeks turn into months, the strictures become harder to tolerate.
Theater and dance hall owners complain about their financial losses.
Clergy bemoan church closures while offices, factories and in some cases even saloons are allowed to remain open.
Officials argue whether children are safer in classrooms or at home.
Many citizens refuse to don face masks while in public, some complaining that they're uncomfortable and others arguing that the government has no right to infringe on their civil liberties.
As familiar as it all may sound in 2021, these are real descriptions of the U.S. during the deadly 1918 influenza pandemic. In my research as a historian of medicine, I've seen again and again the many ways our current pandemic has mirrored the one experienced by our forebears a century ago.
As the COVID-19 pandemic enters its second year, many people want to know when life will go back to how it was before the coronavirus. History, of course, isn't an exact template for what the future holds. But the way Americans emerged from the earlier pandemic could suggest what post-pandemic life will be like this time around.
Sick and tired, ready for pandemic's end
Like COVID-19, the 1918 influenza pandemic hit hard and fast, going from a handful of reported cases in a few cities to a nationwide outbreak within a few weeks. Many communities issued several rounds of various closure orders – corresponding to the ebbs and flows of their epidemics – in an attempt to keep the disease in check.
These social-distancing orders worked to reduce cases and deaths. Just as today, however, they often proved difficult to maintain. By the late autumn, just weeks after the social-distancing orders went into effect, the pandemic seemed to be coming to an end as the number of new infections declined.
People clamored to return to their normal lives. Businesses pressed officials to be allowed to reopen. Believing the pandemic was over, state and local authorities began rescinding public health edicts. The nation turned its efforts to addressing the devastation influenza had wrought.
For the friends, families and co-workers of the hundreds of thousands of Americans who had died, post-pandemic life was filled with sadness and grief. Many of those still recovering from their bouts with the malady required support and care as they recuperated.
At a time when there was no federal or state safety net, charitable organizations sprang into action to provide resources for families who had lost their breadwinners, or to take in the countless children left orphaned by the disease.
For the vast majority of Americans, though, life after the pandemic seemed to be a headlong rush to normalcy. Starved for weeks of their nights on the town, sporting events, religious services, classroom interactions and family gatherings, many were eager to return to their old lives.
Taking their cues from officials who had – somewhat prematurely – declared an end to the pandemic, Americans overwhelmingly hurried to return to their pre-pandemic routines. They packed into movie theaters and dance halls, crowded in stores and shops, and gathered with friends and family.
Officials had warned the nation that cases and deaths likely would continue for months to come. The burden of public health, however, now rested not on policy but rather on individual responsibility.
Predictably, the pandemic wore on, stretching into a third deadly wave that lasted through the spring of 1919, with a fourth wave hitting in the winter of 1920. Some officials blamed the resurgence on careless Americans. Others downplayed the new cases or turned their attention to more routine public health matters, including other diseases, restaurant inspections and sanitation.
Despite the persistence of the pandemic, influenza quickly became old news. Once a regular feature of front pages, reportage rapidly dwindled to small, sporadic clippings buried in the backs of the nation's newspapers. The nation carried on, inured to the toll the pandemic had taken and the deaths yet to come. People were largely unwilling to return to socially and economically disruptive public health measures.
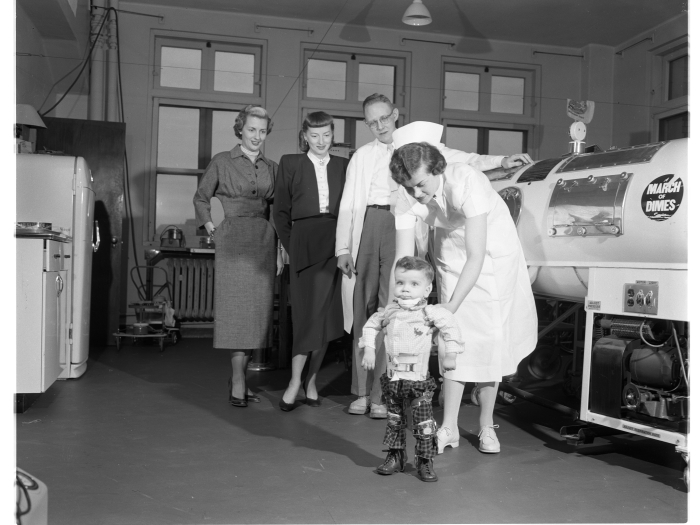
No matter the era, aspects of daily life go on even during a pandemic. Chicago History Museum/Archive Photos via Getty Images
It's hard to hang in there
Our predecessors might be forgiven for not staying the course longer. First, the nation was eager to celebrate the recent end of World War I, an event that perhaps loomed larger in the lives of Americans than even the pandemic.
Second, death from disease was a much larger part of life in the early 20th century, and scourges such as diphtheria, measles, tuberculosis, typhoid, whooping cough, scarlet fever and pneumonia each routinely killed tens of thousands of Americans every year. Moreover, neither the cause nor the epidemiology of influenza was well understood, and many experts remained unconvinced that social distancing measures had any measurable impact.
Finally, there were no effective flu vaccines to rescue the world from the ravages of the disease. In fact, the influenza virus would not be discovered for another 15 years, and a safe and effective vaccine was not available for the general population until 1945. Given the limited information they had and the tools at their disposal, Americans perhaps endured the public health restrictions for as long as they reasonably could.
A century later, and a year into the COVID-19 pandemic, it is understandable that people now are all too eager to return to their old lives. The end of this pandemic inevitably will come, as it has with every previous one humankind has experienced.
If we have anything to learn from the history of the 1918 influenza pandemic, as well as our experience thus far with COVID-19, however, it is that a premature return to pre-pandemic life risks more cases and more deaths.
And today's Americans have significant advantages over those of a century ago. We have a much better understanding of virology and epidemiology. We know that social distancing and masking work to help save lives. Most critically, we have multiple safe and effective vaccines that are being deployed, with the pace of vaccinations increasingly weekly.
Sticking with all these coronavirus-fighting factors or easing off on them could mean the difference between a new disease surge and a quicker end to the pandemic. COVID-19 is much more transmissible than influenza, and several troubling SARS-CoV-2 variants are already spreading around the globe. The deadly third wave of influenza in 1919 shows what can happen when people prematurely relax their guard.
This article is republished from The Conversation under a Creative Commons license. Read the original article.

Explore a variety of health care news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!