A cutting-edge imaging strategy could significantly improve survival rates among patients at risk for liver cancer.
7:00 AM
Author |
Over the past decade, the incidence of hepatocellular carcinoma (HCC) has increased steadily, while most other forms of cancer are on the decline. It's the second-most-common cause of cancer-related deaths worldwide, and the most prevalent primary liver cancer in the United States.
LISTEN UP: Add the new Michigan Medicine News Break to your Alexa-enabled device, or subscribe to our daily audio updates on iTunes, Google Play and Stitcher.
Moreover, the American Cancer Society estimates that there will be 42,000 new cases of primary liver cancer and 30,000 subsequent deaths in 2018 alone.
"The survival rates for patients with HCC remain low because most liver cancers are detected very late," says Anna Lok, M.D., assistant dean for clinical research at the University of Michigan's Department of Internal Medicine. "Effective forms of treatment are no longer an option when the disease is extremely advanced, and that is why early detection for HCC is so important."
Shifting the paradigm of detection
In response to this problem, the National Cancer Institute (NCI) recently funded a new research program at Michigan Medicine to shift the current liver cancer surveillance paradigm and improve early-detection rates in the U.S.
The program, spearheaded by Lok, as well as Grace Su, M.D., and Thomas Wang, M.D., Ph.D., is part of a larger NCI-led initiative to establish a liver cancer consortium by engaging a network of institutions across the country.
"We are very excited to be a part of this consortium," says Su. "Through this collaborative effort, hepatologists and engineers here at U-M can now focus on saving lives by improving liver cancer imaging methodologies."
Improved survival rates
Liver cancer surveillance among high-risk individuals usually leads to earlier diagnoses and improved survival rates among patients. However, this requires several steps, including identification of high-risk patients, compliance with surveillance recommendations, and highly accurate and accessible imaging tools.
Approximately 80 to 90 percent of HCC cases are diagnosed in patients with underlying cirrhosis (scarring) of the liver. For these individuals, the five-year cumulative risk of HCC ranges from 5 to 30 percent, depending on the specific cause. The most common causes of cirrhosis in the U.S. include viral hepatitis (B and C), nonalcoholic steatohepatitis, and alcoholic liver disease.
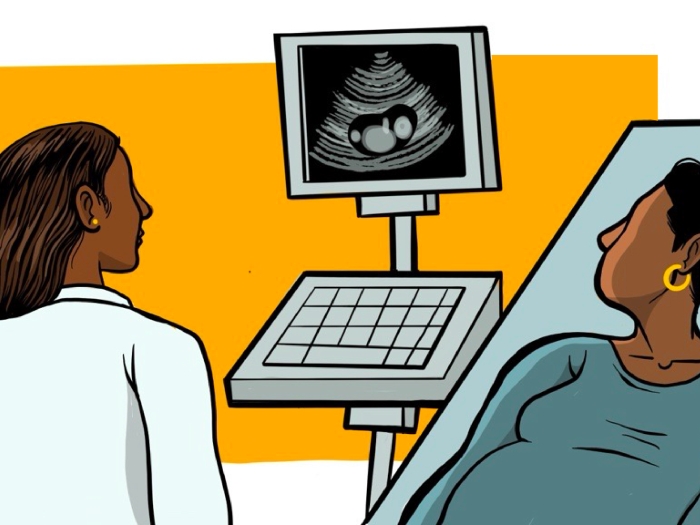
HCC detection relies on the use of ultrasound and blood testing for alpha fetoprotein (AFP). Because of HCC's rapid growth rate, these tests are recommended every six months. This greatly differs from detection methods for many other forms of cancer, which often involve tissue analyses from biopsies.
MORE FROM MICHIGAN: Sign up for our weekly newsletter
"Ensuring that all high-risk patients regularly stick to their six-month surveillance tests can be hard," says Lok. "And it is important to remember that there are limitations with both ultrasound and blood tests — detecting tumor nodules against the background of a nodular cirrhotic liver can be difficult."
When nodules are detected on ultrasound, computed tomography (CT) or magnetic resonance imaging (MRI) scans are performed. Many nodules, particularly when they are small, may not possess all of the characteristics of HCC. Nodules that are not clearly benign or malignant, for example, are considered to be "indeterminate," and management is unclear.
Physicians often recommend that patients with indeterminate nodules undergo repeated CT or MRI scans until it is clear whether they have liver tumors or not. This can directly result in increased levels of patient anxiety, radiation exposure and costs.
More importantly, the diagnosis of HCC may be delayed if the classical features of HCC are subtle.
SEE ALSO: Alcohol-Related Cirrhosis Deaths Skyrocket in Young Adults
"Blood tests for AFP are not always ideal, given that some HCCs do not secrete AFP in the early stages," says Lok. "Moreover, AFP levels can also increase when a patient has cirrhosis, in the absence of HCC."
The team's proposal addresses three distinct approaches to improve early-detection rates for liver cancer through state-of-the-art technology.
The first aim of the program will utilize the electronic medical record (EMR) system to alert providers of high-risk patients who need imaging for surveillance.
"Ultimately, the goal is to translate the EMR algorithm and best practice advisory to other health care systems in the U.S.," says Lok. "It will also send reminders to both patients and physicians when HCC surveillance testing is due, increasing early diagnoses and survival rates."
In the second aim, clinicians will leverage unique "analytic morphomics" software developed at U-M to quantify body dimensions and imaging characteristics of HCC.
SEE ALSO: Video Conferencing Helps PCPs Improve Liver Disease Care, Survival Rates
"Analytic morphomics is a methodology that can be used to precisely measure features within routinely acquired images" (like CT scans), says Su. "This added-value proposition can use computer vision and machine-learning techniques to enhance the use of already existing scans and allow us to extract features that predict HCC earlier than the human eye alone."
The final aim of the program involves the use of molecular imaging that will "tag" specific peptides to visualize the biological processes that drive HCC progression.
"Because the use of molecular imaging is fairly unchartered territory for HCC detection, its potential use is groundbreaking," says Wang. "This has the possibility to open new doors in the realm of liver cancer detection."
For more information about the NCI funding for the liver cancer consortium project led by Drs. Lok, Su and Wang, click here.

Explore a variety of healthcare news & stories by visiting the Health Lab home page for more articles.

Department of Communication at Michigan Medicine
Want top health & research news weekly? Sign up for Health Lab’s newsletters today!